Page 7 - 58peadiatric-surgery-speciality1-7_opt
P. 7
Neonatal Physiology and Transport 9
Table 2.1: Predictable problems in small for gestational age (SGA) and preterm
average for gestational age (AGA) babies.
SGA Pretterm AGA
Lung Pulmonary haemorrhage Hyaline membrane disease Rate
Apnoea + +++
Hypoglycaemia +++ +
Hypeglycaemia + +++
Jaundice + +++
Haemoglobin Polycythaemia Normal
Feeding capacity Normal Reduced
Congenital +++ +
malformations
Mortality +++ Depends upon gestational
age
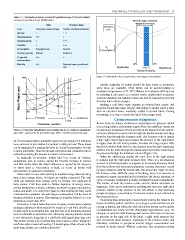
Figure 2.3: Metabolic rates, temperature, and oxygen consumption.
Ideally, surgically ill babies should be kept warm in incubators
Birth Weight (gm) by radiating it into space. In a perfect world, double-lined incubators
when these are available. Most babies can be accommodated in
incubator temperatures of 32–33°C. Babies in incubators still lose heat
would be standard, but radiation losses can also be reduced by covering
the baby with a sheet of paper.
Making a cold baby warm requires an external heat source, and
warming should take place slowly ; attempting to rapidly warm a baby
7
with an electrical heater inevitably results in dermal burns. During
rewarming, it is wise to check the baby’s blood sugar level.
Preterm Postterm
Cardiovascular Adaptation
Gestation (weeks) Before birth, the baby’s circulation is based upon the placenta, which
acts as lung, kidney, and nutrient supply. Thus, the umbilical vessels are
Figure 2.2: Neonatal classification and mortality risk (LGA = large for gestational of paramount importance. Blood arriving at the foetus from the umbili-
age; AGA = appropriate for gestational age; SGA = small for gestational age). cal vein is shunted across the liver through the ductus venosus and away
from the lung through the foramen ovale. The foramen ovale is simply
fat. In premature babies, insensible water loss can amount to 3 ml/kg per a flap “gate” that is held open because the pressure in the right atrium
2
hour, and even in term babies it is around 1 ml/kg per hour. These losses is higher than the left atrial pressure. Because the lungs require little
can be minimised by nursing the baby in a humid environment, but this blood flow before birth, blood is also shunted from the right ventricular
is rarely practicable. Heat loss through convection and conduction can be outflow into the aorta through the ductus arteriosus before returning to
reduced by nursing the neonate in a warm environment. the placenta through the umbilical arteries (Figure 2.4).
In surgically ill neonates, further heat loss occurs in vomitus, When the obstetrician clamps the cord, flow to the right atrium
tachypnoea, and, of course, during the massive increase in surface is reduced and the right atrial pressure falls. There is a simultaneous
area that occurs when the baby’s abdomen is opened by the surgeon, increase in left atrial pressure in response to increased pulmonary blood
or where there is evisceration at birth, as occurs in babies with flow that follows the decreased pulmonary vascular resistance caused
gastroschisis or ruptured exomphalos. by lung expansion with the first breath. This allows the “gate” to close
Babies who become cold must try to maintain temperature by using the foramen ovale. With the onset of breathing, there is an increase in
their scarce energy stores, but these are rapidly exhausted. The well peripheral oxygen concentration that stimulates the ductus arteriosus to
child can replenish these energy stores by feeding. The surgically ill close, a muscular contraction probably mediated through prostaglandin.
baby cannot. Cold then leads to further depletion of energy stores, The closure of both the foramen ovale and the ductus arteriosus are
protein breakdown, acidosis, sclerema, increased oxygen consumption, temporary. They can be reopened by anything that increases right atrial
sepsis, and death. It is clear from Figure 2.3 that keeping the baby warm pressure relative to the pressure in the left atrium or that decreases
minimises the metabolic rate and oxygen consumption, but the zone of peripheral oxygen concentration. Permanent closure is not achieved in
thermal neutrality is narrow. Hypothermia is formally defined as a core the neonatal period.
temperature lower than 36°C. Reopening these temporarily closed shunts restores the infant to the
Prevention is much better than cure. Keeping a baby warm requires foetal circulatory pattern, but there is no longer a placenta that can act
strategies different to those required to warm up a cold baby. A baby can as lung or kidney, and unless the adult circulatory pattern can be rapidly
be kept warm by enveloping him, and his head, in an insulating material re-established, the infant will die. Pulmonary hypertension, seen, for
such as a blanket or aluminium foil, obviously ensuring that the airway example, in neonates with diaphragmatic hernia, will cause an increase
is not obstructed; doing this to a cold baby will simply keep him cold. in pressure on the right side of the heart, a right atrial pressure that
The mother’s body is an excellent heat source and so-called “kangaroo” will exceed left atrial pressure, reopening of the foramen ovale, and
5
4
care also aids in maternal bonding. It would appear that, at least in the ultimately reduction in peripheral arterial oxygen concentration and
short term, fathers are capable substitutes. reversal of ductal closure. Without a placenta, this circulatory pattern
6